Erectile dysfunction (ED) affects men of all ages and rarely has just one cause. The most common physical drivers are poor cardiovascular health, diabetes, high blood pressure, obesity, and low testosterone — many of which overlap. Lifestyle habits like smoking, heavy drinking, inactivity, and chronic stress play a significant role too, especially in younger men. Psychological factors such as anxiety and depression are just as real, and often intertwined with physical ones. Importantly, ED can be an early warning sign of underlying heart disease. The good news: it’s treatable, and the same habits that protect your heart also protect your sexual health.
If you’ve been Googling this at midnight, you’re not alone. Erectile dysfunction is one of the most common sexual health concerns men bring to their doctor — and one of the most under-discussed.
The good news is that understanding what’s driving it is usually the first step toward doing something about it. ED isn’t a single condition with a single cause. It’s more like a symptom — one that can point to several different things happening in the body or mind. For some men it shows up once during a stressful stretch of life and never again. For others it’s persistent and tied to something more systemic. Knowing the difference matters.
Why Erections Are More Complicated Than They Seem
An erection depends on a surprisingly coordinated chain of events. It starts in the brain with arousal, travels through nerve signals, triggers increased blood flow to the penis, and relies on blood vessels staying open and healthy long enough to maintain firmness.
Disrupt any one of those steps — whether it’s circulation, nerve function, hormones, or your mental state — and you can run into problems. That’s why ED can have so many different causes, and why a doctor will often want to investigate rather than just hand over a prescription.
Medical Conditions That Raise Your Risk
Certain health conditions are strongly and consistently linked to erectile dysfunction. If you have any of the following, it’s worth having a conversation with your doctor about how it might be affecting your sexual health.
Heart Disease and Circulatory Problems
Here’s something most men don’t know: the blood vessels in the penis are smaller than the ones that supply the heart. That means circulation problems often show up as ED before they show up as chest pain. Persistent erectile dysfunction can actually be an early warning sign of cardiovascular disease — which is one reason doctors take it seriously.
Diabetes
Men with diabetes are at significantly higher risk of ED, and often experience it earlier in life. Chronically elevated blood sugar can damage both the nerves and the blood vessels involved in achieving an erection. The longer diabetes goes unmanaged, the greater that risk becomes.
High Blood Pressure
Hypertension wears down blood vessel walls over time. That reduces the quality of circulation throughout the body including to the penis. It’s worth noting that some blood pressure medications can also contribute to ED, so this is worth discussing with your prescribing physician.
Obesity
Carrying excess weight affects erectile function in several ways at once: it increases cardiovascular risk, lowers testosterone levels, and promotes inflammation. Men who are obese are roughly three times more likely to experience ED compared to men at a healthy weight.
Low Testosterone
Testosterone drives libido and plays a supporting role in erectile function. Low levels can dampen sexual desire and make arousal more difficult. It doesn’t always cause ED directly, but it often contributes, especially in men over 40.
Lifestyle Factors Worth Paying Attention To
Some of the most significant ED risk factors aren’t diagnoses but habits. And the flip side of that is that they’re also among the most modifiable.
Smoking
Smoking damages blood vessel walls and reduces circulation throughout the body. The evidence linking smoking to ED is strong and consistent. Men who quit often report improvements in sexual function — another reason to add to an already long list.
Heavy Alcohol Use
A drink or two probably isn’t going to cause problems. But regular heavy drinking interferes with nerve signaling involved in arousal and can suppress testosterone over time. Acute alcohol intoxication — the well-known “whiskey dick” phenomenon — reflects the same underlying nerve disruption.
Suggested Read: The Impact of Smoking and Alcohol on Male Sexual Health
Physical Inactivity
Regular exercise supports cardiovascular health, helps maintain a healthy weight, and can actually boost testosterone levels. A sedentary lifestyle does the opposite. You don’t need to train like an athlete — even consistent moderate exercise makes a measurable difference.
Poor Sleep
Most testosterone production happens during deep sleep. Chronically poor sleep — whether from insomnia, sleep apnea, or just not getting enough hours — can noticeably affect hormone levels and energy. Men with untreated obstructive sleep apnea have higher rates of ED than those without it.
Chronic Stress
Stress triggers a hormonal cascade that’s not friendly to sexual function. Cortisol — the primary stress hormone — suppresses testosterone and keeps the nervous system in a heightened state that isn’t conducive to arousal. Men under prolonged stress often notice changes in their sex drive and performance before other symptoms appear.
The Psychological Side of ED
This piece gets underestimated. Mental and emotional factors are significant contributors to erectile dysfunction — not as a moral failing or weakness, but as straightforward physiology. Anxiety activates the sympathetic nervous system (the “fight or flight” response), which actively works against arousal.
Common psychological contributors include:
- Performance anxiety — a self-reinforcing cycle where fear of not performing creates the very problem you’re afraid of
- Depression, which often reduces libido and physical sensation
- Relationship tension or communication issues
- General life or work-related stress
In many cases, ED involves both physical and psychological factors intertwined. Addressing one without the other often produces incomplete results.
How ED Risk Changes With Age
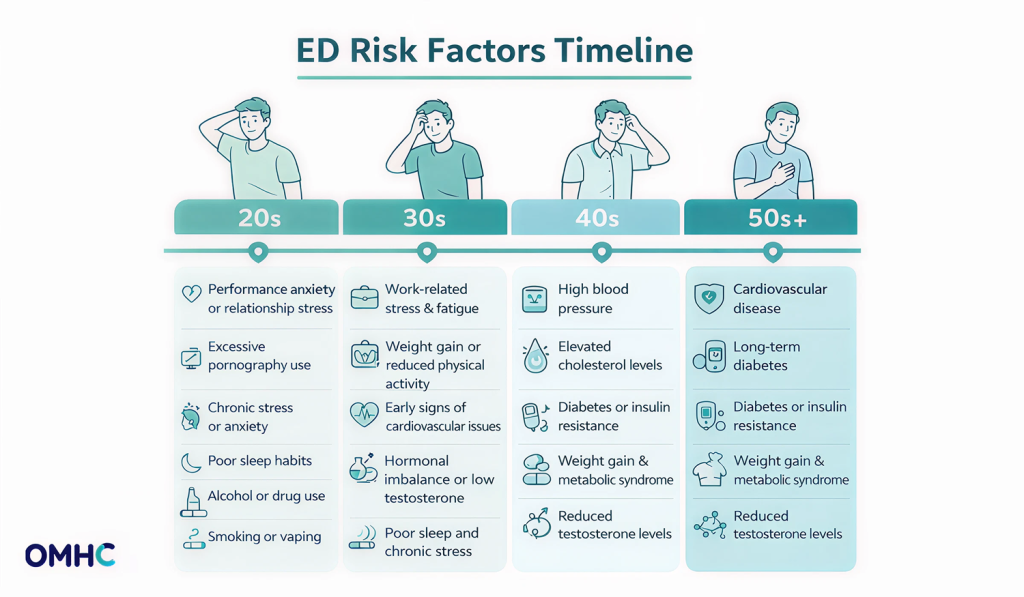
ED isn’t just an older man’s problem, but the driving factors do shift across different decades of life.
In Your 20s
ED in younger men tends to be psychological or lifestyle-driven. Performance anxiety is especially common in men who are new to sexual relationships or who’ve developed unrealistic expectations from pornography. Substance use — alcohol, cannabis, recreational drugs — also plays a significant role in this age group.
In Your 30s
This is when physical factors start creeping in alongside psychological ones. Work stress and fatigue become more prominent. Weight gain — from reduced activity and busier schedules — starts affecting cardiovascular health and hormone levels. Some men in their 30s are dealing with early blood pressure or metabolic issues without knowing it yet.
In Your 40s
ED becomes more common in this decade, with physical causes taking the lead. High blood pressure, elevated cholesterol, insulin resistance, and declining testosterone levels all become more prevalent. This is also when medication side effects can enter the picture — several commonly prescribed drugs, including certain antidepressants and blood pressure medications, can affect erectile function.
In Your 50s and Beyond
Circulatory changes and chronic health conditions are the dominant drivers here. Atherosclerosis (narrowing of the arteries), long-term diabetes, and hormonal shifts all become more significant. That said, men in their 50s and beyond can and do treat ED effectively — age is a risk factor, not a life sentence.
Suggested Read: Sexual Health Tips for Men Over 50
Early Signs That Are Worth Noticing
ED doesn’t usually arrive overnight. Most men notice gradual changes first — and those early signals are worth paying attention to rather than dismissing.
- Difficulty maintaining an erection firm enough for sex
- Reduced or absent morning erections
- Noticeably decreased interest in sex
- Erections that take longer to develop or feel less firm than they used to
- Inconsistent sexual performance that’s becoming more frequent
None of these in isolation necessarily means something is seriously wrong. But if several are occurring regularly, that’s worth raising with a doctor.
Can You Actually Prevent ED?
There are risk factors that are difficult or impossible to reverse. But a meaningful portion of ED risk is modifiable, and the same habits that protect your heart tend to protect your sexual health too. Evidence-backed protective habits include:
- Regular aerobic exercise (even 30 minutes, most days)
- Maintaining a healthy weight
- Not smoking — and if you do, quitting
- Limiting alcohol to moderate levels
- Getting enough consistent sleep
- Managing chronic conditions like diabetes and hypertension
- Finding sustainable ways to manage stress
When to Talk to a Doctor
Occasional erection difficulties are normal. Stress, fatigue, and alcohol can all cause a one-off issue. But if it’s happening regularly, or if you’ve noticed a gradual decline over weeks or months, that’s worth investigating. The same is true if you’re experiencing low libido, persistent fatigue, or mood changes alongside it.
ED is often a treatable condition. But more importantly, it can sometimes be the first visible sign of something like cardiovascular disease or diabetes, conditions that are much better managed early. A conversation with a men’s health physician can help sort out what’s actually driving the issue and what to do about it.
Most Frequent Questions and Answers
ED Risk Factor FAQs
What is the most common cause of erectile dysfunction?
Circulatory problems are the single most common physical cause. Anything that impairs blood flow, including heart disease, high blood pressure, and diabetes-related vascular damage, can reduce the quality and reliability of erections. That said, psychological factors are a close second, particularly in younger men.
Can lifestyle changes actually improve ED?
Yes, in many cases. Exercise, weight loss, quitting smoking, and reducing alcohol have all shown measurable improvements in erectile function in clinical studies. The degree of improvement depends on what’s driving the ED. Lifestyle changes work best when lifestyle factors are the primary cause.
Is erectile dysfunction always related to aging?
No. While the prevalence of ED increases with age, it’s not an inevitable part of getting older. Men in their 20s and 30s can and do experience it, typically due to stress, psychological factors, or lifestyle habits. Men in their 60s and 70s can also have healthy sexual function.
Can low testosterone cause erectile dysfunction?
Low testosterone more directly affects libido than the mechanics of an erection, though the two are connected. Men with low testosterone often notice reduced desire for sex, which naturally reduces arousal and contributes to ED. It’s rarely the sole cause, but it’s commonly part of the picture.

Dr. Derek McLellan is a family physician with six years of focused experience in men’s health. He is a recognized provider of medical care in the evaluation and treatment of male sexual health and hormone-related conditions in Ottawa.
His clinical practice includes the assessment and management of erectile dysfunction, testosterone deficiency, and other men’s health concerns. With a background in family medicine, Dr. McLellan approaches patient care through comprehensive evaluation, evidence-based treatment planning, and ongoing clinical monitoring.